Axillary Access, ECMO, Escalation Therapy, Unloading, Surgical Applications
Expert Strategies for Management of Post-Cardiotomy Cardiogenic Shock
Scott Silvestry, MD, of AdventHealth in Orlando leads a panel discussion on management of post-cardiotomy cardiogenic shock (PCCS). Panel members include Zain Khalpey, MD, PhD, FETCS, FACS, from Northwest Medical Center in Tucson; Masahiro Ono, MD, PhD, from Methodist Hospital in San Antonio; Danny Ramzy, MD, from Cedars-Sinai in Los Angeles; and Deane Smith, MD, from NYU Langone Health in New York City.
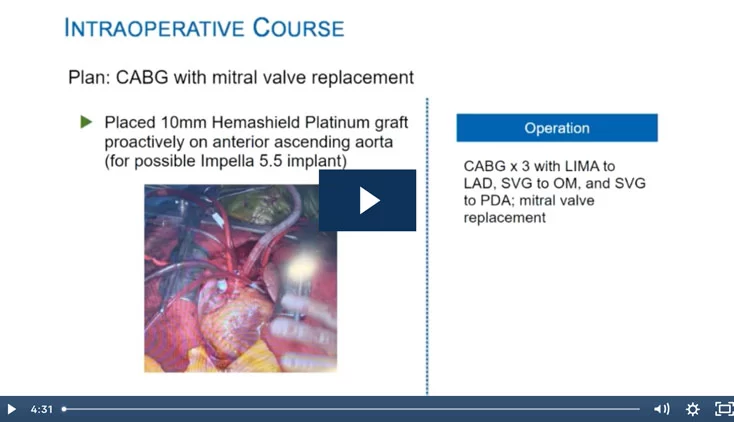
After briefly defining post-cardiotomy shock, Dr. Silvestry and the panel discuss topics including identification of PCCS risk factors and the importance of understanding the intraoperative picture to make the most appropriate treatment decisions. They explore PCCS treatment options, notably the Impella 5.5® with SmartAssist® heart pump, implanted either centrally or through the axillary artery, and acknowledge that support may require several steps and an experienced multidisciplinary team with a variety of available tools.
Dr. Silvestry acknowledges that physicians who work in heart failure often approach assist devices and unloading differently than surgeons who tend to be most comfortable increasing drugs and adding an intra-aortic balloon pump (IABP), noting “and these can be dangerous ways of approaching this.”
Dr. Khalpey emphasizes the importance of pre-emptively identifying patients prior to surgery and having an Impella® heart pump ready, “because sometimes going on ECMO isn’t the holy grail that the surgeons think. You’ve got to decompress… and offloading the left ventricle actually takes you a long way.”
Dr. Ramzy describes that at his referral center for advanced heart failure and shock they often receive patients from hospitals that do not have the tools to provide sufficient support for patients who develop shock. “The devices are available here. So if we recognize shock, we treat early. We don’t go with inotropes and then say ‘we’ll see how they do and then come back’ … We go with the definitive therapy first and that really has affected outcomes.” He emphasizes, “the greatest impact on survival, is having the strategy ahead of time, even in the emergency cases.”
Dr. Ono states that at his transplant shock center he often receives calls from surgeons who cannot wean patients from bypass in the OR. He explains that his facility comprehensively assesses patient risk and attempts to consult early on cases with low EF or other significant comorbidities to prepare an exit strategy of LVAD, durable LVAD, or transplant. He also notes that they try to limit use of post-cardiotomy ECMO due to significant mortality. Later in the discussion, Dr. Silvestry presents ECMO data and discusses which patient types may be most likely to benefit from ECMO.
“The best treatment for post-cardiotomy cardiogenic shock, I think, is prevention,” Dr. Smith emphasizes. “As much as we can figure out ahead of time who the patients are at risk, and design a strategy, whether it’s going to be the right ventricle, you know, left ventricle, or whatever it may be that’s going to be the problem, and be prepared for it, I think is tremendously valuable.”
“Every center must have a strategy for cardiogenic shock; must have at least a device for cardiogenic shock,” Dr. Ramzy concludes. “And if they’re not able to keep and manage these patients, they must have a strategy for transfer or a relationship with a hospital that can manage cardiogenic shock.”
NPS-1691