Acute Kidney Injury (AKI), Clinical Research & Data, Complete Revascularization, Cost-Effectiveness, IABP, Impella Education, Safety & Efficacy
What is the PROTECT Series?

The PROTECT Series of FDA clinical studies includes PROTECT I6, PROTECT II RCT2 (the only FDA randomized, controlled trial ever conducted for hemodynamically supported high-risk PCI), and PROTECT III. Abiomed initiated the PROTECT Series in 2006 with the PROTECT I study and conducted the PROTECT II RCT from 2007 to 2010. The ongoing PROTECT III prospective, single-arm, FDA post-approval study began in 2017.
The PROTECT Series has enrolled 1,366 patients as of July 2019 with PROTECT I (N=20), PROTECT II RCT (N=448) and PROTECT III (N=898, as of July 2019). At the Transcatheter Cardiovascular Therapeutics (TCT) conference in September 2019, Jeffrey Popma, MD, of Harvard Medical School and Beth Israel Deaconess Medical Center, presented an interim analysis of the high-risk PCI patients treated through July 2019. The Impella® heart pump is the most studied mechanical circulatory support device and has been included in 8 clinical guidelines and more than 550 peer-reviewed publications.
William O’Neill, MD, medical director of the Center for Structural Heart Disease at Henry Ford Hospital and a principal investigator on the PROTECT Series states, “The totality of clinical data in favor of Impella supported high-risk PCI allows interventional cardiologists to be confident they are using the optimal treatment and technologies to help achieve complete revascularization in a single setting, improve procedural hemodynamic stability, and improve patient quality of life.”
What is PROTECT II?
PROTECT II was a landmark prospective, multicenter, randomized, controlled trial of hemodynamic support with Impella 2.5® versus intra-aortic balloon pump (IABP) in patients undergoing nonemergent high-risk percutaneous coronary intervention (PCI). The study was designed to assess whether an Impella-supported high-risk percutaneous revascularization strategy would result in better outcomes than a revascularization strategy with IABP support.1
PROTECT II was conducted at 112 sites in the United States, Canada, and Europe. Between November 27, 2007 and December 6, 2010, 452 patients, 18 years of age and older, were enrolled in the PROTECT II study.1 PROTECT II was the basis of the U.S. Food and Drug Administration’s (FDA) decision to grant Impella its highest level of regulatory approval as safe and effective for high-risk PCI procedures. Since that approval, additional data has been collected in the USPella registry and cVAD Study® and continues to be collected in the PROTECT III study.
The primary endpoints of the PROTECT II study, as per the study design, were 30-day and 90-day incidence of major adverse events (MAEs). Secondary endpoints included in-hospital efficacy and safety endpoints consisting of efficacy of hemodynamic support assessed by maximal decrease in cardiac power output (CPO) from baseline, creatinine clearance change from baseline 24 hours post-PCI, device failure assessed as Impella flow < 1L/min for > 5 minutes at performance level 5 (out of 9) or higher, and rate of in-hospital MAEs.1
What patient population was studied in PROTECT II?
Inclusion criteria
The PROTECT II study patient population consisted of patients requiring hemodynamic support during nonemergent, high-risk PCI. These patients required either:1
- PCI on an unprotected left main or last patent coronary vessel with left ventricular ejection fraction (LVEF) ≤ 35%, or
- PCI for 3 vessel disease with LVEF ≤ 30%
Exclusion criteria
Major exclusion criteria included:1
- Myocardial infarction (MI) with persistent elevation of cardiac enzymes
- Left ventricular thrombus
- Platelet count ≤ 75,000/mm3
- Creatinine ≥ 4 mg/dL (patients already on dialysis were eligible)
- Severe peripheral vascular disease that precluded passage of the Impella 2.5® catheter or IABP
Baseline characteristics
Baseline characteristics were similar between groups, except for a higher incidence of heart failure and previous coronary artery bypass grafting in the Impella 2.5 arm.1 Average patient baseline characteristics:
- 67 ± 11 years of age
- Predominantly (~80%) male in each group
- Highly symptomatic (66% in NYHA class III or IV)
- 87% had heart failure
- 51% had diabetes mellitus
- Presented with an average LVEF of 24% ± 6%
- SYNTAX score of 30 ± 15
- STS mortality score of 6% ± 6%
- STS combined mortality and morbidity score of 30% ± 15%
Two thirds of the patients were deemed inoperable by site surgical consultants
Only one third of this population had received implantable defibrillators despite the low LVEF
What is the difference between the intent-to-treat (ITT) and per protocol (PP) patient populations in PROTECT II?
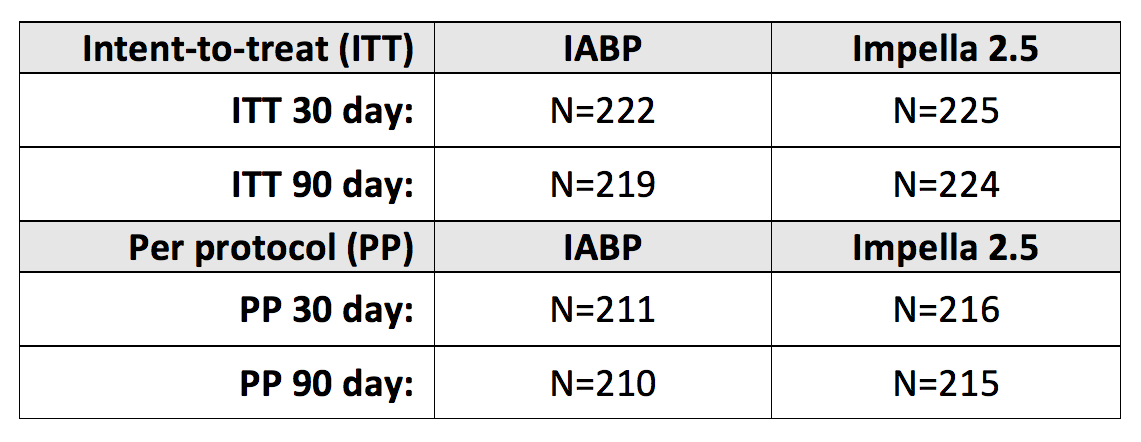
The intent-to-treat (ITT) population in the PROTECT II study included all consented randomly assigned patients undergoing high-risk PCI in the study, regardless of the protocol compliance and duration of follow-ups. This included 448 patients (232 in the IABP arm and 225 in the Impella 2.5 arm). Of these patients, 427 met the protocol eligibility criteria and were included in the per protocol (PP) population (211 in the IABP arm and 216 in the Impella 2.5 arm).1
The following list identifies those patients who did not meet the protocol eligibility requirements and the reasons they did not:
- 4 patients did not meet the criteria of ejection fraction (EF) ≤ 35%
- 4 patients did not have 3-vessel disease (3VD) or unprotected left main disease (ULM)
- 3 patients had active myocardial infarction (MI)
- 3 patients had severe peripheral vascular disease (PVD) or aortic stenosis (AS)
- 2 patients had platelets < 70,0000
- 2 patients withdrew consent post PCI
- 1 patient had creatinine > 4
- 1 patient was lost to follow-up post discharge
- 1 PCI was performed after the study stopped
The number of patients at 90-day follow-up in each group differed from 30-day follow-up.1
What were the primary endpoints of the PROTECT II study?
The study design established 2 primary endpoints in the PROTECT II study:
- Composite rates of intra- and post-procedural major adverse events (MAEs) at discharge or 30-day follow-up, whichever was longer
- Composite rates of intra- and post-procedural major adverse events (MAEs) at 90 days
At the time the PROTECT II study was designed, there were no prospective comparative studies with respect to outcomes for devices providing support during high-risk procedures.1 Because these types of patients had not previously been studied, the design was MACCE plus additional endpoints added by the FDA for further insight into potential adverse events associated with these devices in clinical practice. The trial was not designed, and therefore, not statistically powered, to show a difference in mortality or MACCE alone.
The composite primary endpoint components included 10 individual adverse event components:1
- All-cause death
- Q-wave MI (development of new, pathological Q waves in ≥ 2 continuous leads) or non–Q-wave MI (defined as creatinine kinase-MB (CK-MB) isoenzyme ≥ 3 times the upper limit of the normal (ULN) range within 72 hours of the procedure or ≥ 2 times ULN range beyond 72 hours post-procedure.) Cardiac troponin values were used if CK-MB isoenzyme was not available.
- Stroke or transient ischemic attack (TIA)
- Any repeat revascularization procedure (PCI or coronary artery bypass grafting (CABG))
- Need for a cardiac or a vascular operation (including a vascular operation for limb ischemia)
- Acute renal insufficiency
- Severe intraprocedural hypotension requiring therapy
- Cardiopulmonary resuscitation or ventricular tachycardia requiring cardioversion
- Aortic insufficiency
- Angiographic failure of PCI
What were the results in PROTECT II?
The primary endpoint of 30-day MAE in the PROTECT II study occurred in 34.3% of the per protocol (PP) patients in the Impella 2.5 arm compared with 42.2% of PP patients in the IABP arm (P=0.092). However, as shown in the figure below, the 90-day MAE rate was significantly lower in the Impella 2.5 arm compared with the IABP arm (40.0% versus 51.0%, P=0.023), yielding a relative risk reduction of 22%.1
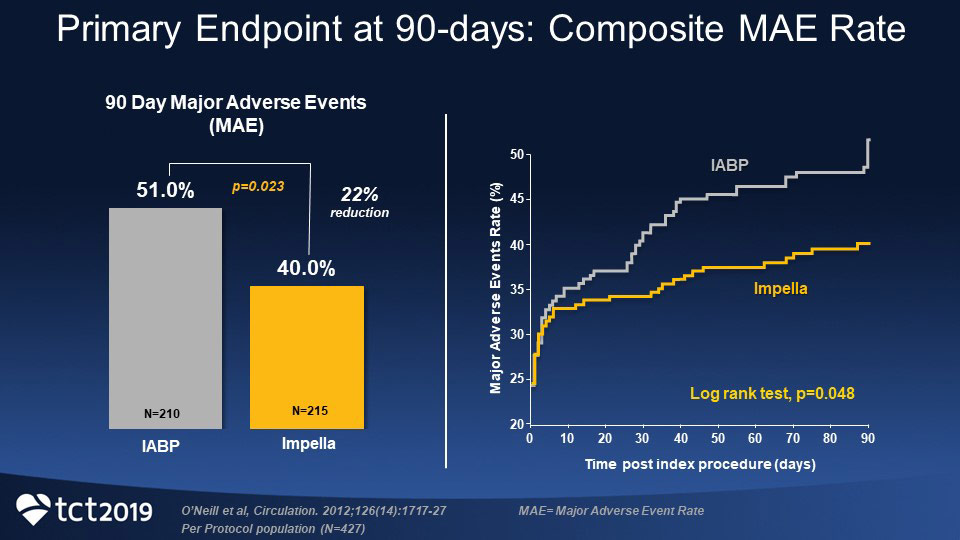
Although there was no difference in in-hospital death, stroke, MI, or the composite of death/stroke/MI between Impella 2.5 and IABP, fewer irreversible MAEs of death/stroke/MI (and of death/stroke/MI/repeat revascularization occurred after hospital discharge in the Impella 2.5 arm compared with the IABP arm.1

At 90 days, there were also fewer repeat revascularization events in the Impella 2.5 arm compared with the IABP arm in both hierarchical (3.7% versus 8.1%, P=0.055) and nonhierarchical (6.0% versus 12.4%, P=0.024) analyses.1
Procedural characteristics
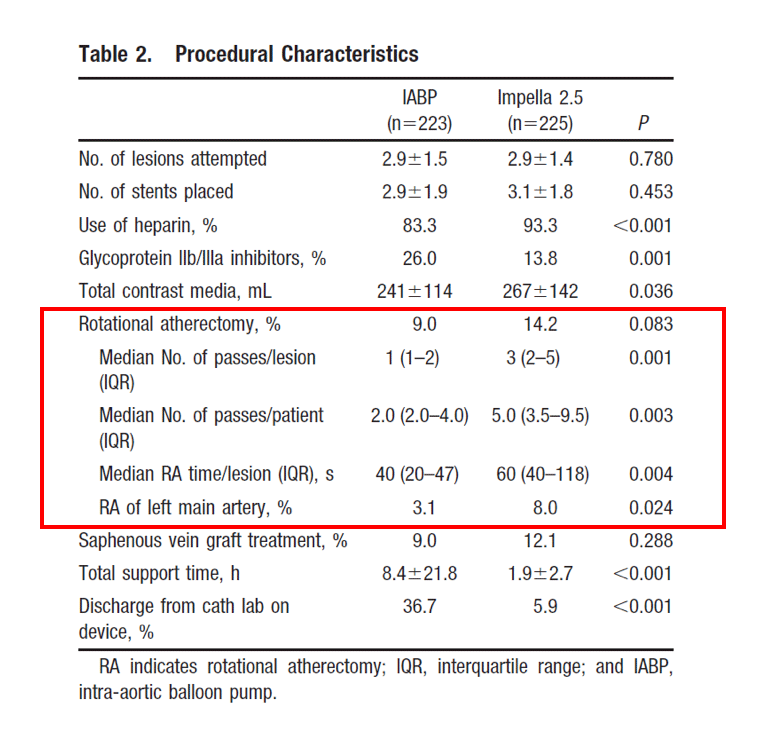
In both study arms, more lesions were attempted than originally planned by the interventionalists (2.9 ± 1.5 for IABP; 2.9 ± 1.4 for Impella 2.5). While the number of attempted lesions and deployed stents (2.9 ± 1.9 for IABP; 3.1 ± 1.8 for Impella 2.5) were similar between the two groups, the proportion of patients treated with three or more stents was slightly higher in the Impella 2.5 arm.1
There were significant differences between the study arms with respect to the use of adjunctive therapies.1
- Rotational atherectomy use tended to be more frequent in the Impella 2.5 arm (14.2% compared with 9% for IABP, p=0.083)
- The use of rotational atherectomy was also more vigorous in the Impella arm, with more runs and longer durations
- Rotational atherectomy was also more frequently performed in unprotected left main lesions in the Impella 2.5 arm
- The volume of contrast used was significantly greater in the Impella 2.5 arm (267 ± 142 mL versus 241 ± 114 mL for IABP, p=0.036)
- Patients randomly assigned to IABP had longer duration of support compared with those in the Impella 2.5 arm (8.4 ± 21.8 hours versus 1.9 ± 2.7 hours, p<0.001)
- Glycoprotein IIb/IIIa receptor antagonists were used less frequently in the Impella 2.5 arm (13.8% of patients compared to 26% in the IABP arm, p=0.001)
Was there a difference in MACCE—death, stroke, large MI, and repeat revascularization—in PROTECT II?
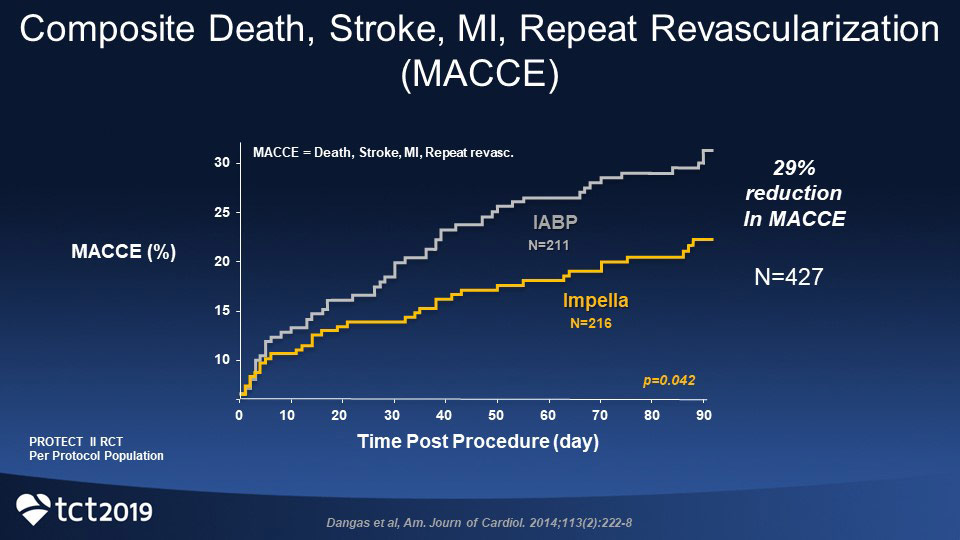
In 2014, Dangas et al. published in The American Journal of Cardiology an evaluation of the PROTECT II study results with “more prognostically relevant composite endpoints,” specifically major adverse cardiac and cerebrovascular events (MACCE). MACCE was defined as all-cause mortality, myocardial infarction, stroke or transient ischemic attack (TIA), or any repeat revascularization procedure (PCI or CABG). MI was defined as the development of new Q-waves or CK-MB elevation ≥ 8x ULN within 72 hours post-PCI for periprocedural myocardial infarction (pMI), or as ≥ 2x the upper limit of normal (ULN) beyond 72 hours of the PCI for spontaneous MI (sMI), the latter representing the same criteria in the original PROTECT II protocol.
Dangas et al. wrote that small to moderate elevations of troponin or CK-MB biomarkers after PCI have a benign clinical course. While at the time of the PROTECT II trial design, the universal definition of MI had a cutoff of ≥ 3x ULN for cardiac biomarker elevation, numerous studies since then have documented the limitations of this definition and this threshold in determining outcome measures in clinical trials. Large multicenter have confirmed that at least a 10x elevation of CK-MB after PCI was required for a long-term effect on mortality to be seen.7 For this reason, Dangas et al. reexamined the outcomes of the PROTECT II study using the more prognostically relevant 8x ULN definition of myocardial infarction and strengthened their analyses by including multivariable testing for predictors of cardiovascular adverse events.2
The principle results from Dangas et al. were that in the high-risk population that underwent PCI, use of Impella compared with IABP resulted in significantly lower MACCE rates at 90 days when using “a more clinically relevant definition” of periprocedural myocardial infarction (pMI). At 90 days, the rate of MACCE in the Impella group was 22% compared with 31% in the IABP group (p=0.034)—a 29% reduction in MACCE.2 Most events occurred after hospital discharge.2

Why was PROTECT II discontinued early?
Study design background
The PROTECT II study independent data safety monitoring board (DSMB) monitored the safety trends on a monthly basis and provided oversight of data at 25% and 50% of planned study enrollment. The DSMB was tasked with one formal preplanned interim analysis of the first 50% of patients (n=327). This analysis was designed to evaluate the feasibility of the study with a futility guideline based on the conditional power at the interim mark, which was the probability of observing a statistically significant treatment effect at the end of a trial, on the true treatment trends for the remaining 50% patients to be enrolled. A conditional power <40% at interim was the cutoff at which the DSMB could recommend stopping the study for futility.1
Decision to discontinue
After review of the available interim data (n=327), the DSMB recommended the early discontinuation of the study for futility based on the observed conditional power of the 30-day results of the first 327 patients and the assumed similar trend for the remaining 327 patients to be included in the study. When the executive committee accepted the recommendation and study enrollment ceased (December 6, 2010), an additional 125 patients had been enrolled beyond the 327 patient halfway point to which the DSMB had limited the interim analysis. Therefore, the total final cohort increased to 452 patients—69% of the planned enrollment. Of these, three withdrew consent (IABP arm) and one died (Impella 2.5 arm) before undergoing PCI. Thus, the primary analysis of the full cohort included all 448 intent to treat (ITT) patients randomly assigned to either Impella 2.5 (n=225) or IABP (n=223). The prespecified per-protocol (PP) population included 427 patients who met the protocol-mandated eligibility criteria (216 for Impella 2.5 and 211 for IABP).1
Study limitation
When the DSMB recommended early discontinuation of the study, an analysis of the significant learning curve had not been completed. A marked improvement for Impella-supported patients treated in the last half of the trial was noted, and an analysis after the first case and a year by year assessment all demonstrated a learning effect on safety.1
In addition, endpoints in the PROTECT II study as reported were driven by periprocedural myocardial infarction (pMI), many of which were characterized by small to moderate elevations in CK-MB or troponin, which in most studies have not been found to have prognostic relevance. Dangas et al. in their analysis of the PROTECT II study published in 2014, wrote: “The impact of prognostically important large MIs compared with small elevations of cardiac enzymes as part of the main efficacy endpoint would be expected to be especially relevant in a high-risk cohort such as the patients enrolled in PROTECT II.”2
Dangas et al. used the more “prognostically relevant” definition of MI: development of new Q-waves or CK-MB elevation ≥ 8x ULN within 72 hours post-PCI for periprocedural MI (pMI) (rather than ≥ 3x ULN used in original PROTECT II definition), or as ≥ 2x the upper limit of normal (ULN) beyond 72 hours of the PCI for spontaneous MI, the latter representing the same criteria in the original PROTECT II protocol. They write that when the definition of MI “was restricted to only include large pMIs, the type which has been associated with subsequent mortality, use of Impella rather than IABP was found to be an independent predictor of freedom from MAE and MACCE, with pMI rates being similar in both groups.”2
Did the extent of revascularization affect outcomes in PROTECT II?
Analysis of the PROTECT II study data by Kovacic et al. revealed that Impella maintains patient hemodynamics allowing for more complete revascularization. Results showed that patients supported with Impella consistently experienced significantly smaller maximum decreases in mean arterial pressure, regardless of whether PCI involved 1, 2, or 3 vessels. In fact, Impella protected patients experienced the least drop in arterial pressure relative to the IABP when 3 vessels were treated. When 3 vessels were treated, the maximum decrease in mean arterial pressure was nearly 19% in the IABP arm compared with < 8% in the Impella arm (p=0.026).3

In 2019 David Burke, MD, and Duane Pinto, MD, published an analysis of PROTECT II data demonstrating that Impella benefit was more pronounced with extensive revascularization. Revascularization was characterized by the change in myocardial jeopardy score (MJS) pre- and post-PCI. The scoring system assigned 1 point for each of 11 potential obstructions prior to PCI and subtracted the point if the obstruction was cleared. Patients with an MJS change of 2 or lower were considered to have undergone “limited” revascularization while a change of 3 to 11 was considered “extensive” revascularization.4
With limited revascularization, there was virtually no difference in cumulative incidence of MACCE (35.1% Impella versus 32.2% IABP, P=0.867). However, with extensive revascularization the difference in cumulative incidence of MACCE at 90 days was 15.0% Impella versus 29.3% IABP, P=0.006.

Multiple studies have revealed that more complete revascularization leads to reduced adverse events. Data from William O’Neill, MD, presented at TCT 2013, along with other studies show that extensive revascularization is important because it correlates with improved patient outcomes. In the PROTECT II study, more extensive revascularization led to lower MACCE. With 1 vessel treated, the MACCE rate was 33.8% at 90 days in both IABP and Impella arms. The MACCE rate fell to 23.3% with 2 vessels treated, and 17.0% with 3 vessels treated.

What about vascular complications with the larger Impella sheath compared with IABP?
Despite the larger device diameter and intraventricular placement, treatment with Impella in the PROTECT II study did not result in more vascular repair operations than IABP. In addition, it did not result in aortic or mitral valve dysfunction or left ventricular injuries.2
In the 90-day per protocol population in PROTECT II, the incidence of vascular complications in the IABP arm was 1.9% compared with 1.4% in the Impella arm.1 Dangas et al. writes that this was due to the device safety features, careful operator training, and protocol-derived patient screening.2
What did we learn from PROTECT II?
Procedural benefits
The procedural benefits of hemodynamically Protected PCI with Impella are fewer hypotensive events, higher cardiac power output, and facilitation of more extensive atherectomy.
- Half as many hypotensive events per patient occurred in the Impella 2.5 arm compared with the IABP arm (0.45 versus 0.96, p=0.001). This was a 53% reduction in hypotensive events, which were defined as MAP<65 mmHg.

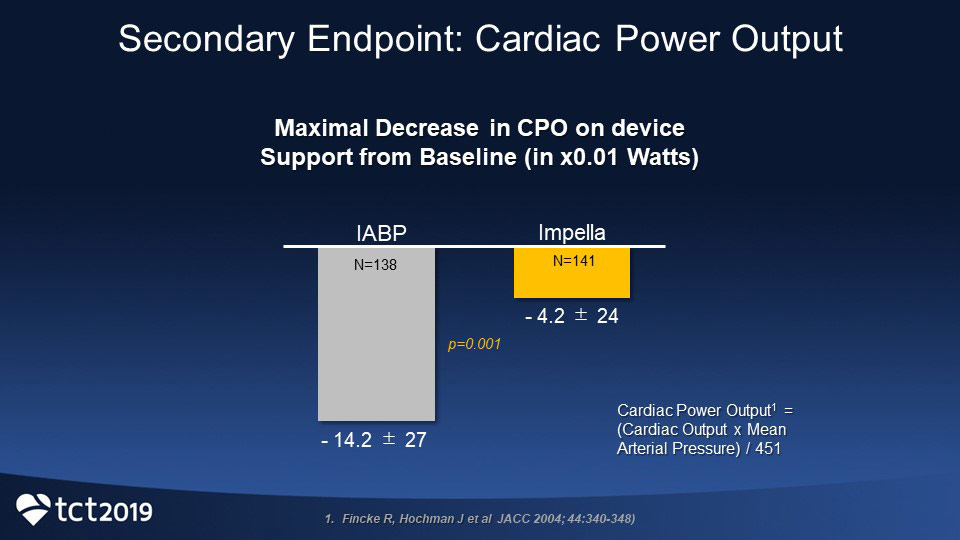
- Cardiac power output (CPO) was calculated to account for systemic blood flow and maintenance of physiologically appropriate blood pressure during the procedural ischemic times. As determined by the maximal drop in CPO from baseline, Impella 2.5 provided better hemodynamic support than IABP during these high-risk procedures (-4.2 ± 24 vs -14.2 ± 27 W, P=0.001).
- Impella facilitated more extensive atherectomy. Among Impella patients with STS ≥ 10, 27% had atherectomy, which is approximately 3 times the rate of atherectomy use in the rest of the population.
Clinical benefits
The clinical benefit of Protected PCI with Impella was a reduction of major adverse events (MAE) post-discharge accompanied by an improvement in ventricular function and heart failure symptoms.
For both intent to treat (ITT) and per protocol (PP) populations, patients treated with Impella 2.5 experienced fewer MAEs over the course of the study compared with those treated with IABP. Most of the differences in patient MAE outcomes occurred out of the hospital. These new events were overt and mainly driven by death or rehospitalizations for MI, stroke, and repeat revascularization in a patient population that was event free at discharge.1
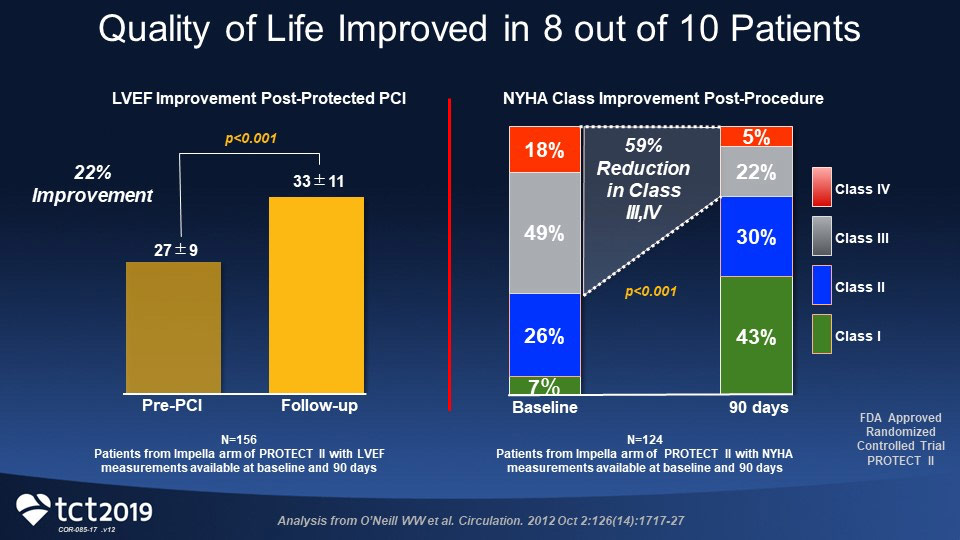
In both the IABP and Impella 2.5 arms of the PROTECT II study, patient cardiac function and functional status improved significantly after revascularization. At 90-day study exit follow-up, there was an average 22% relative increase in LVEF from baseline (P>0.001) and a 59% improvement in NYHA functional class III/IV (P≤0.001).
These post-discharge clinical benefits were more pronounced in patients who underwent more complete revascularization with Impella support.
Are there studies of the cost-effectiveness of Impella?
Published studies have demonstrated the cost-effectiveness of Impella support for patients undergoing high-risk PCI and also in the emergent setting for patients in cardiogenic shock.
Is Impella cost-effective in high-risk PCI?
In 2013, Gregory et al. demonstrated that Impella was cost effective over the long term in the first economic analysis in the United States to compare resource utilization costs for Impella versus IABP in patients requiring acute hemodynamic support. Results reported from this study show that index hospitalization costs were $33,684 for IABP versus $47,667 for Impella.
However, both readmission length of stay and costs were lower in the Impella cohort (5 days, $11,007) than in the IABP cohort (7 days, $21,824). In addition, in the Impella cohort the major adverse event (MAE) rate was 22% lower (40.0% for Impella versus 51.0% for IABP, P=0.023) and the major adverse cardiac and cerebrovascular events (MACCE) rate was 29% lower than in the IABP cohort.5
When considering the cost effectiveness of a treatment regimen, it is important to consider the short-term costs of procedures as well as the long-term costs for ongoing care with respect to improvement in objective clinical outcomes. Gregory et al. used clinical and economic data from the PROTECT II randomized controlled trial (RCT) as well as a simulation analysis of the longer-term value of Impella, using a probabilistic Markov model, to estimate the incremental cost-effectiveness of Impella versus IABP in terms of quality-adjusted life-years (QALY).5
Gregory et al. wrote that in the case of Impella utilization, “the acquisition cost is significantly greater than standard-of-care devices and must be assessed in a context of potentially decreasing the frequency of serious major AEs (adverse events) and lowering the rates of readmission over a reasonable time horizon.”5 Conclusions in this paper state that for high-risk patients with advanced heart failure undergoing PCI, Impella “reduced major adverse events, critical care and readmission length of stay, and readmission cost over the 90-day EOC (episode of care), and was determined to be cost-effective over the long-term.”5
When considering a multiyear extended timeline for judging the value of Impella in high-risk PCI, Gregory et al. state, “our study suggests that the incremental expenditure per QALY gained is cost-effective and well within the willingness-to-pay range that is widely accepted for other advanced cardiovascular technologies.”5 Specifically, the authors state that the estimated 10-year incremental cost for Impella relative to IABP in high-risk PCI was $10,241, with an estimated incremental gain of 0.26 QALYs. They write, “This equates to an ICER [incremental cost-effectiveness ratio] of $39,389 per QALY, which is below the widely accepted willingness-to-pay thresholds of $50,000 and $100,000 for other advanced cardiovascular technologies.” This 10-year ICER reflects the long-term value of Impella and is derived from an increase in quality of life for patients with Impella, supplemented by an extension of life expectancy driven by reduced MACCE. The authors note that this data reveals that the acquisition cost of Impella begins to dissipate shortly after the initial 90 days and that inpatient costs begin to moderate annually due to the reduction in MACCE in Impella-supported patients.
Gregory et al. conclude that the short-term and longer-term finding they present “have implications for medical coverage decisions and underscore a value proposition that health plans and accountable care organizations should carefully consider during the technology assessment process.”
Is Impella cost-effective in cardiogenic shock?
Research published by Maini et al. in 2014 adds to existing evidence that pVADs have a beneficial impact on the economic as well as clinical outcomes of AMI patients with cardiogenic shock (CS). Maini et al. conclude, “for patients in CS requiring emergent hemodynamic support, pVAD therapy offers a less invasive alternative that can be deployed sooner, resulting in better outcomes, shorter LOS, lower costs and with no incremental cost, and a survival benefit when compared to traditional surgical hemodynamic support alternatives."
PVAD therapy (and Impella 2.5 in particular) is emerging as a dominant strategy for this challenging patient population.”8
This study by Maini et al. compared the cost-effectiveness of pVAD circulatory support in patients with AMI complicated by cardiogenic shock to the cost-effectiveness of circulatory support provided by traditional surgical hemodynamic support alternatives (i.e., ECMO and extracorporeal LVADs). This study also presented a case study from PinnacleHealth in which a formal protocol was implemented for the timely use of Impella for this patient population, providing important national research showing a significant survival benefit when Impella was placed prior to revascularization.8
Patients who received a pVAD had a higher survival rate at discharge compared with traditional surgical hemodynamic support alternatives (56% vs 42%, p<0.001). Among the PinnacleHealth patients, the survival rate was even higher at 60% of patients treated with Impella between 2009 and 2011 (p=0.056) and in 2012 both the discharge and 30-day follow-up survival rates improved to 67%.8
Improvement in survival was achieved with a strong trend toward reduced length of stay (LOS) (13.2 days for patients receiving a pVAD compared with 17.9 days, p=0.055) and a lower cost of the index admission ($90,939 vs $144,257, p<0.0001). The PinnacleHealth LOS was 66% lower than the surgical hemodynamic support alternatives (17.9 days vs 6.0 days for Impella, p=0.003).8
What is Protect III?
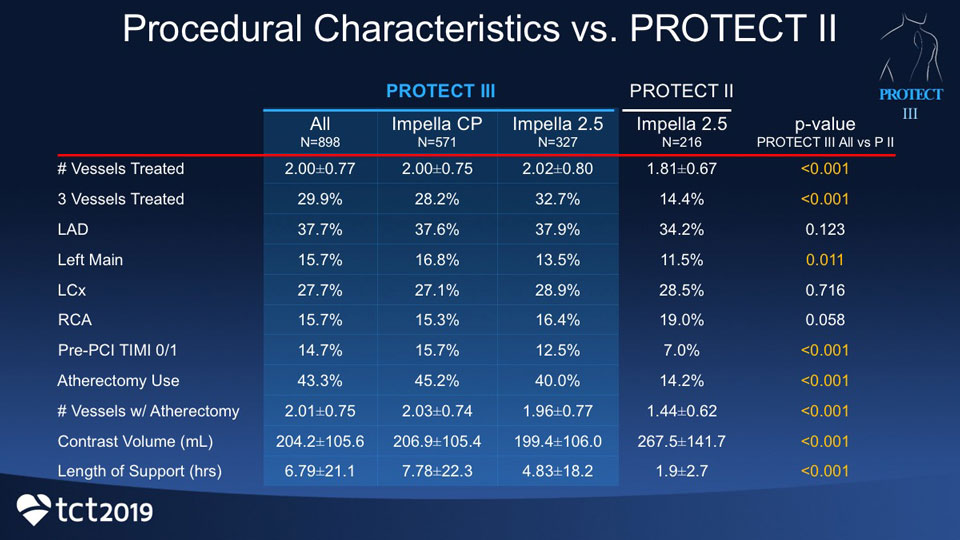
PROTECT III is an ongoing, prospective, single-arm, FDA post-approval study for the post-marketing approval (PMA) of Impella 2.5® and Impella CP® in high-risk PCI. PROTECT III follows the PROTECT II randomized controlled trial (RCT). As of July 2019, the PROTECT III study includes 898 patients enrolled at 45 sites in the United States since March 2017.
At the Transcatheter Cardiovascular Therapeutics (TCT) conference in September 2019, Jeffrey Popma, MD, of Harvard Medical School and Beth Israel Deaconess Medical Center, announced findings from an interim analysis of 898 patients. PROTECT III demonstrates a reduction in the primary endpoint of major adverse cardiac and cerebrovascular events (MACCE) at 90 days with Impella-supported protected PCI, compared to the PROTECT II study. MACCE includes death, stroke, myocardial infarction (MI), and repeat procedures.
How does the patient population in PROTECT III compare to PROTECT II?
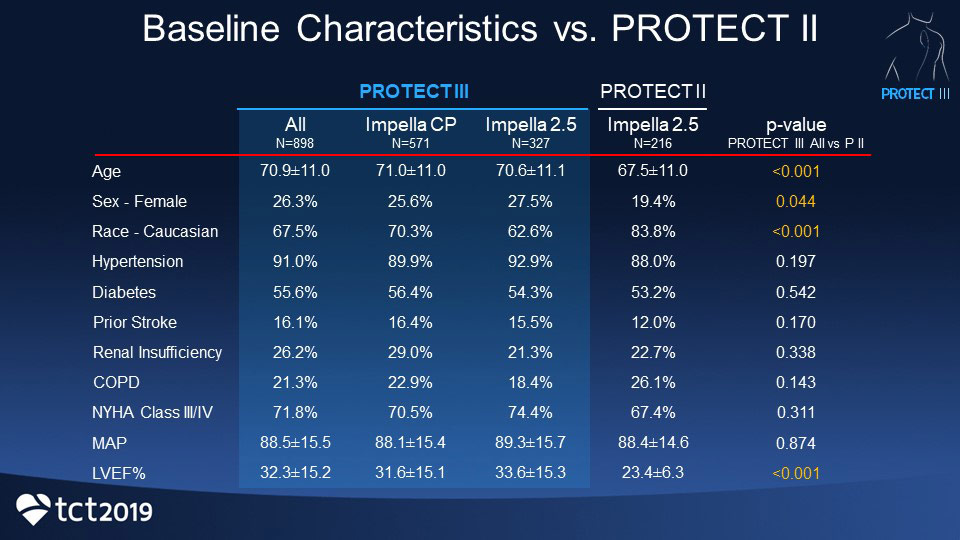
Patients in the PROTECT III study differed from patients in the PROTECT II study:
- Statistically older (71 years versus 67.5)
- More women (26% versus 19.4%)
- More non-Caucasians (33% versus 26.2%)
- Received longer support (6.79 versus 1.9 hours of support)
- Had more complex procedures with more vessels treated (43.3% atherectomy versus 14.2%; 29.9% had 3 vessels treated versus 14.4%)
What were the interim findings for PROTECT III?
Although PROTECT III patients had, according to Dr. Jeffrey Popma, “more complex anatomic lesions” (the number of vessels treated per patient in the PROTECT III study was higher and the amount of atherectomy used was significantly higher), patients in PROTECT III had better outcomes than patients in PROTECT II.
The 90-day MACCE rate in the PROTECT III study is lower than the intra-aortic balloon pump (IABP) control arm from the PROTECT II study. The composite MACCE rate in the IABP arm was 31% compared to the Impella 2.5 and Impella CP arm at 16.8% (p<0.0001).
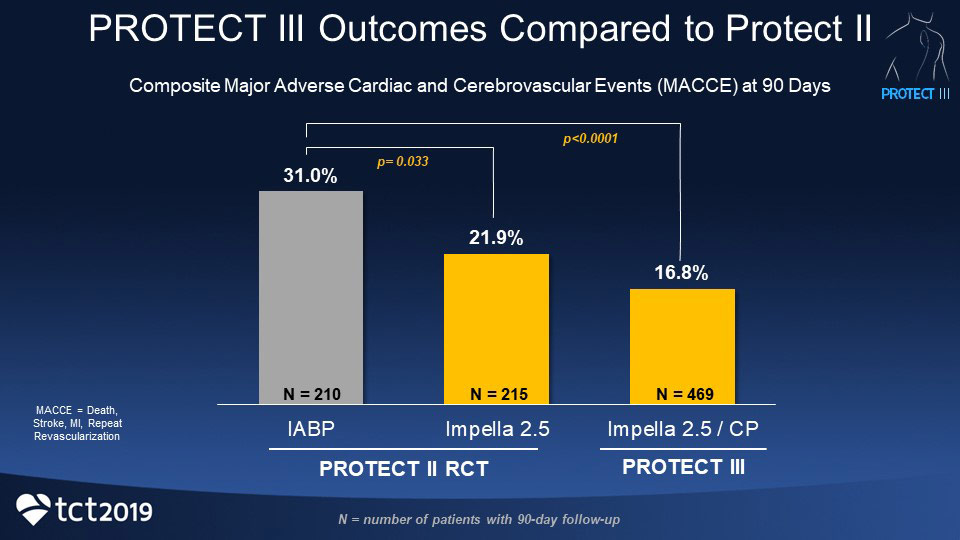
“Based on the learnings from the PROTECT studies, decisions to provide hemodynamic support during PCI should be made in the context of providing complete revascularization and patient outcomes should include in-hospital and out-of-hospital improvement,” Dr. Popma states. “Prior studies have demonstrated it is important to achieve complete revascularization because it can result in a 30-50% reduction in MACCE, compared to incomplete revascularization.”
What acute kidney injury (AKI) data is available from the PROTECT Series of studies?
High-risk PCI patients face elevated risk of acute kidney injury (AKI) due to high levels of contrast and long procedures. Additionally, chronic kidney disease is a common comorbidity. According to a NCDR Cath PCI Registry Study of 985,737 patients, in-hospital mortality for patients with AKI is 10% and escalates to 34% if dialysis is required.
In the PROTECT III study, a sub-study (N=106) of patients were evaluated for acute kidney injury rate and compared to a propensity matched control group (N=106). Results indicate a reduction in any acute kidney injury as well as lower severity of kidney injury in patients treated with Impella in PROTECT III.
Additionally, multiple studies with Impella have measured the AKI rate based on predicted AKI risk factors, including contrast volume. These include:
- Circulation, 2012 -The PROTECT II RCT found Impella patients had statistically higher contrast volume than the IABP arm (267 mL vs. 241 mL, p=0.04), but a numerically lower rate of acute renal dysfunction at 30 days and 90 days (p=0.792 and p=0.776, respectively), showing a decoupling of contrast volume from renal dysfunction.
- Circulation Research, 2017 - Flaherty, et al. identified a 6-fold reduction in AKI requiring dialysis in Impella supported patients compared with patients who did not receive Impella support (p=0.031).
- Catherization and Cardiovascular Interventions, 2019 – Flaherty et al. found that compared to a predicted rate of 22% (using the Mehran risk score), only 5% of Impella supported patients developed AKI (exclusively stage 1) at 48 hours, representing a 77.6% lower AKI risk (p<0.0001).

What can we conclude, thus far, from the PROTECT Series of clinical studies?
“We are in a very good place now, with our understanding and clinical evidence base for high-risk PCI with left ventricular support,” Dr. Jeffrey Popma stated in his presentation of the current clinical evidence for Protected PCI with left ventricular support at TCT 2019.
- The “high-risk” indication for PCI is founded on a procedural benefit of hemodynamic stability enabling a more thorough revascularization and leading to a post-discharge clinical benefit of reduced adverse events and improved cardiac function.
- Decisions to provide hemodynamic support during PCI should accordingly be made in the context of providing complete revascularization and evaluated based on improvement in outcomes out of hospital.
- In the post-approval era, compared to the PROTECT II study, the PROTECT III study patients are older, include more women, and receive more complex procedures, yet 90-day MACCE is lower.
- Emerging data validated in the multicenter cVAD Study® indicate a potential additional benefit in these patients to reduce the risk of acute kidney injury.
References
- O’Neill, W.W., et al. (2012). Circulation, 126(14), 1717-1727.
- Dangas, G.D., et al. (2014). Am J Cardiol, 113(2), 222-228.
- Kovacic, J.C., et al. (2015). J Interv Cardiol, 28(1), 32-40.
- Burke, D.A., et al. (2019). JACC Cardiovasc Interv, 12(19), 1985-1987.
- Gregory, D., et al. (2013). Am Health Drug Benefits, 6(2), 88-99.
- Dixon, S.R., et al. (2009). JACC Cardiovasc Interv, 2(2), 91-96.
- Moussa, I.D., et al. (2013). J Am Coll Cardiol, 62(17), 1563-1570.
- Maini, B., et al. (2014). Catheter Cardiovasc Interv, 83(6), E183-E192.
IMP-1022